I motivi per cui considero questo articolo scientifico pubblicato nel 2009 una pietra miliare su questo argomento sono molteplici: l'autorevolezza degli Autori, l'ampia casistica di oltre 3000 pazienti, l'aver valutato anche la lieve discesa delle tonsille cerebellari (Low-Lying Cerebellar Tonsils) e non solo la discesa delle tonsille cerebellari tali da configurare la malformazione di Chiari tipo I (CM1), l'aver correlato le varie discese delle tonsille cerebellari alla sindrome del midollo ancorato e alla sindrome del midollo ancorato occulto.
Faccio presente che il trattamento chirurgico della sindrome del midollo ancorato e della sindrome del midollo ancorato occulto è stato eseguito in ANESTESIA GENERALE con la sezione del FILUM TERMINALE INTRADURALE.
Il mio intervento chirurgico mininvasivo in ANESTESIA LOCALE della sezione EXTRADURALE del FILUM TERMINALE, di cui parlerò più avanti qui e in altre pagine del sito web, è stato pubblicato successivamente nel 2018, anche se lo eseguo dal 2010.
© Copyright 2020 Vanni VERONESI. All rights reserved.
Informativa sulla Privacy (ITALIANO) / Privacy Policy (ENGLISH)Informativa sui Cookies (ITALIANO) / Cookies information (ENGLISH)
The minimally invasive surgical technique under local anaesthesia for the section of the extradural tract of the filum terminale can only have a possible skin infection at the level of the surgical incision as a complication.
To avoid this possibility, the protocol provides antibiotic prophylaxis in the operating room before the start of the surgery.
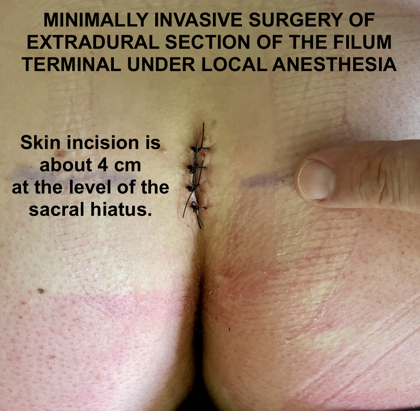
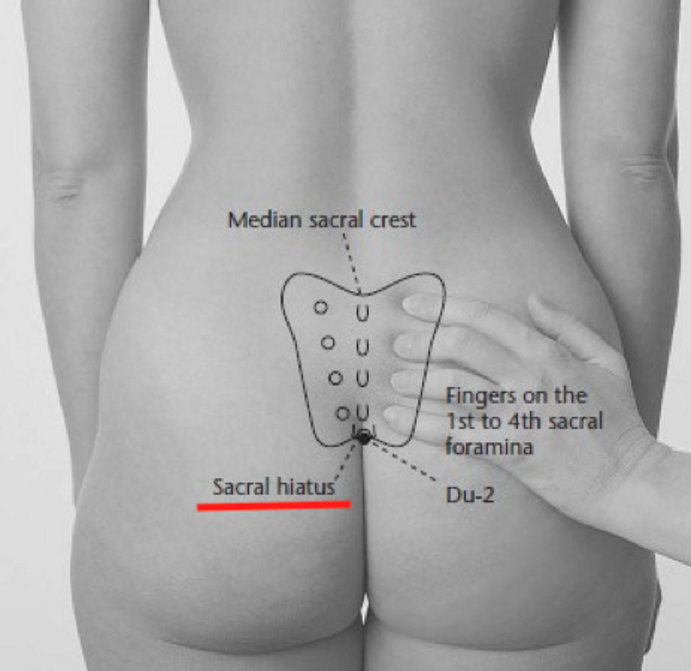
The skin cut is about 4 cm long and is made at the level of the sacral hiatus.
No bone tissue is removed from the vertebrae or sacrum.
The posterior sacrococcygeal ligament is removed, and using the microsurgical technique, which involves using the operating microscope, the extradural filum terminale is isolated and cut.
For a video description of the technique CLICK HERE.
Having neither meninges nor nervous structures in the operating field, there can be no neurological damage or the appearance of meningitis.
The surgery takes about 25 minutes, and you can walk again after 60 minutes.
The patient is discharged from the hospital the day after the surgery.
The surgical intervention for anatomical reasons does not foresee the opening of the meninges; therefore, with this minimally invasive surgical technique, there are no conditions for the complication of the re-tethering described in the surgical interventions with traditional surgery under general anaesthesia.
INNOVATIVE MINI-INVASIVE SURGERY UNDER LOCAL ANESTHESIA FOR THE SECTION OF THE EXTRADURAL FILUM TERMINALE
ADVANTAGES
- LOCAL ANESTHESIA
- SMALL CUT OF THE SKIN (see box below)
- SHORT DURATION OF THE INTERVENTION
- NO NEUROLOGICAL COMPLICATIONS
- AFTER THE SURGERY, ONLY ONE HOUR OF BED REST
- ONLY ONE DAY OF HOSPITALIZATION
- THERE ARE NO ANATOMICAL CONDITIONS FOR RETETHERING
A small skin cut is sufficient to carry out the mini-invasive surgical approach to the sacral spinal canal through the sacral hiatus

INFORMATIONAL VIDEO
SECTIONING EXTRADURAL (EXTERNUM)
FILUM TERMINALE IN LOCAL ANESTHESIA:
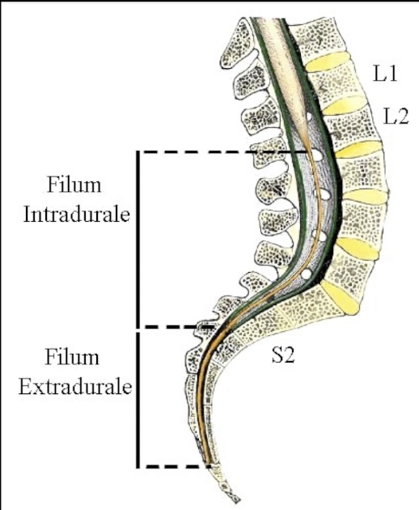
- ANATOMY
- SURGICAL TECHNIQUE
- POSTOPERATIVE COURSE
FOR A SCIENTIFIC AND INFORMATION PURPOSE
CLICK BELOW TO EXIT THIS WEB SITE AND CONNECT TO YOUTUBE CHANNEL BY VANNI VERONESI M.D. AND SEE THE VIDEO

Innovative minimally invasive surgery of EXTRADURAL section of the filum terminale. Review the scientific literature in human and veterinary medicine.
Data updated to 30 March 2025.
Only five scientific papers describe the innovative surgery of the EXTRADURAL section of the filum terminale for the treatment of tethered cord syndrome and occult tethered cord syndrome.
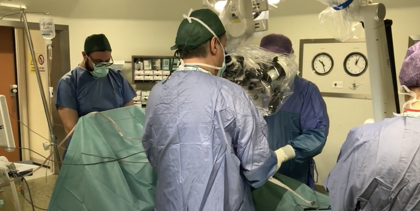
EXTRADURAL FILUM TERMINALE SECTIONING IN LOCAL ANESTHESIA
SURGICAL VIDEO
The operating microscope is used in the central part of the surgery for the section of the extradural filum terminale.
CLICK BELOW TO EXIT THIS WEB SITE AND CONNECT TO YOUTUBE CHANNEL BY VANNI VERONESI M.D. AND SEE THE VIDEO (dialogues in Italian and Portuguese).

TRADITIONAL SURGERY IN GENERAL ANESTHESIA FOR THE SECTION OF THE INTRADURAL FILUM TERMINALE
Traditional surgery of the intradural section of the filum terminale requires general anaesthesia for about one to two hours.
Risk of this traditional surgery in general anaesthesia including permanent bowel and bladder deficits, new neurological deficits.
Risk of CSF (cerebrospinal fluid) leak, pseudomeningocele, cauda tethering, conus medullaris tethering and repeated surgeries to above. Risk of wound healing problems and meningitis with associated morbidity and mortality.”
The classic surgical approach involves:
- the removal of the back part of the vertebrae;
- the opening of the meninges;
- identification of the intradural filum terminale between the nerve roots of the cauda equina (and verification using electrostimulation to avoid cutting the nerve roots with consequent neurological damage).
The duration of the intervention is approximately 60-90 minutes.
Before starting the surgery, under general anaesthesia, time is added to prepare for intraoperative electrophysiological monitoring.
The length of the skin cut is usually about 8-12 cm.
After surgery, bed rest in the prone position is provided for one to two days.
The discharge is foreseen three or four days after the intervention.
Cases of re-tethering due to adhesions of previously open meninges have been described with this technique.
Using the endoscope reduces the length of the skin cut and the invasiveness but does not significantly modify the other aspects and complications of the traditional technique.

LAST UPDATE 14th SEPTEMBER 2024

© Copyright 2020 Vanni VERONESI. All rights reserved.